If you’re generally healthy — balanced diet, regular exercise, good hydration, and stress management — yet you consistently wake up with under-eye puffiness and dark circles, the explanation often lies not in what you do during the day, but in what happens (or doesn’t happen) at night. Insufficient sleep duration, delayed bedtimes, and evening screen exposure are among the most common — and overlooked — disruptors of facial fluid balance and appearance.
The periorbital region (the skin around the eyes) is uniquely vulnerable to these disruptions. It is the thinnest skin on the face (approximately 0.5 mm), contains minimal subcutaneous fat, and is supported by loose connective tissue that readily accumulates fluid. As a result, even small shifts in fluid dynamics, vascular tone, or inflammation become visibly apparent here — often before they appear elsewhere on the face.
Here are typical examples of morning periorbital edema (puffiness) with accompanying dark circles following insufficient or poorly timed sleep:
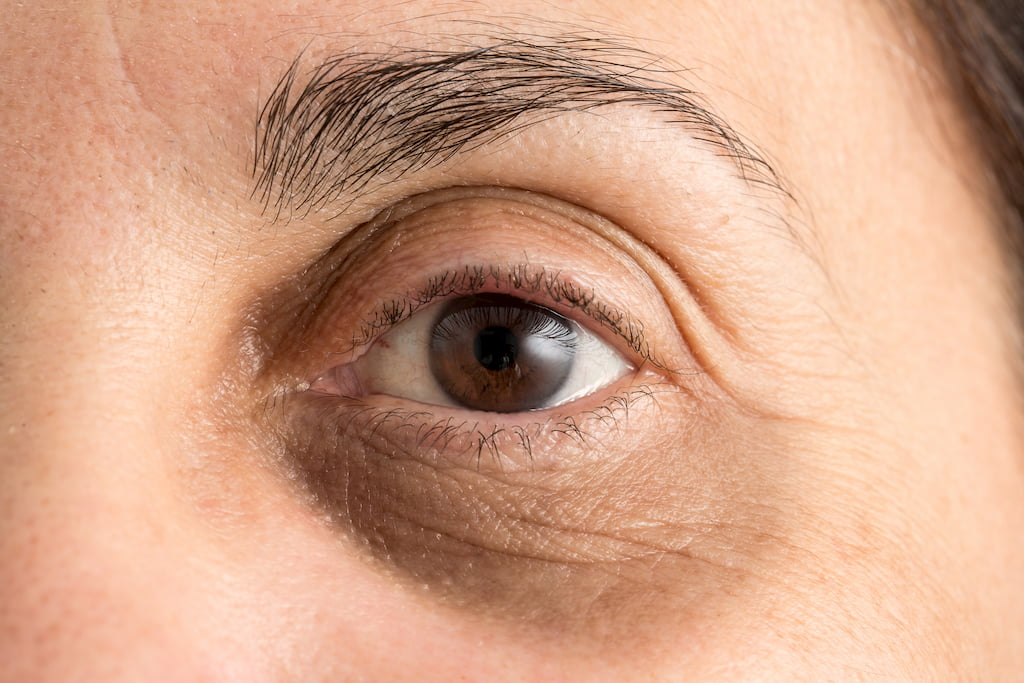
Core Mechanism: Sleep Deprivation Activates the Stress Axis and Disrupts Fluid Homeostasis
Insufficient sleep duration (consistently less than 7–9 hours) and delayed sleep onset act as physiological stressors. Both activate the hypothalamic-pituitary-adrenal (HPA) axis, leading to elevated cortisol secretion that often persists into the following day.
Cortisol plays a key role in fluid and electrolyte regulation through several mechanisms:
- Enhanced renal sodium reabsorption (via mineralocorticoid receptor activation)
- Increased extracellular fluid volume
- Osmotic shifts that favor interstitial fluid accumulation
During prolonged recumbency (lying flat overnight), this excess fluid gravitates toward dependent and loosely supported tissues — particularly the under-eye area — resulting in prominent morning periorbital edema.
Here is a simplified schematic of the HPA axis and its role in the stress response:
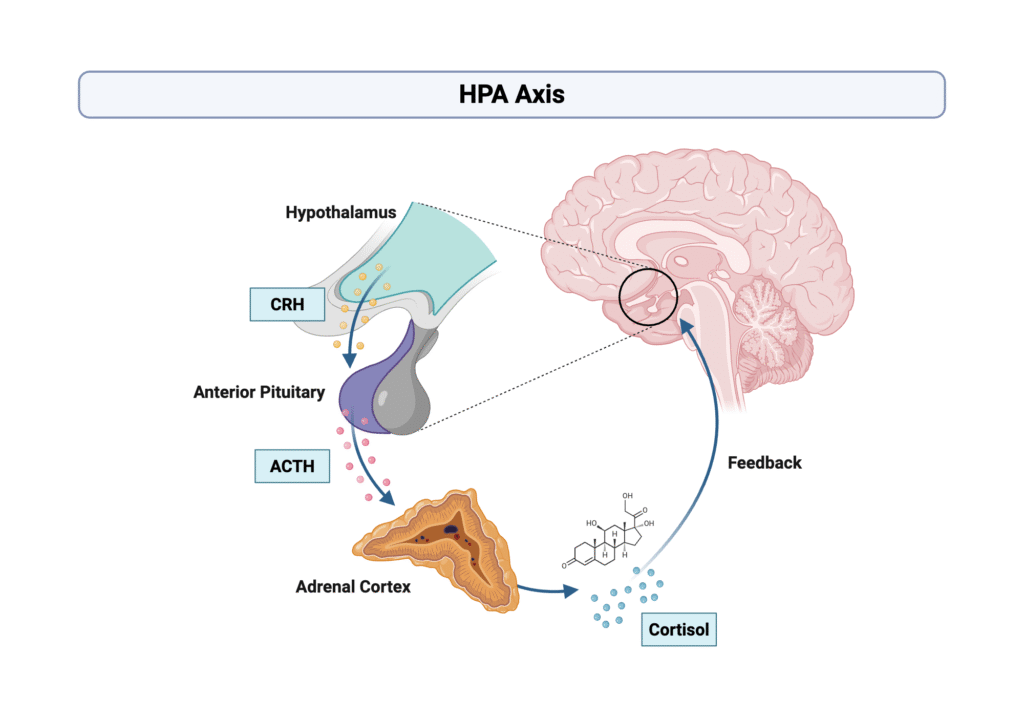
Clinical studies consistently demonstrate that partial or total sleep restriction elevates evening and next-day cortisol levels, disrupts its normal diurnal decline, and promotes systemic fluid retention.
You can explore more on how chronic stress affects the face and body in our related article:
The hidden ways stress wears down your body, mind, and skin.
For additional scientific background, see:
National Institutes of Health (NIH) on sleep deprivation and stress
Medscape overview of the Impact of Sleep Deprivation on Hormones and Metabolism
Late Bedtimes and Evening Blue Light Exposure Compound the Problem
Going to bed late — even when total sleep duration appears adequate — misaligns the circadian rhythm and reduces time spent in deeper, restorative sleep stages. This impairs the body’s natural overnight regulation of fluid balance and lymphatic clearance.
Compounding this effect, nighttime screen use (phones, tablets, laptops) exposes the eyes to blue light (peak wavelengths ~450–480 nm), which strongly suppresses melatonin production. Research, including systematic reviews and Harvard-affiliated studies, shows that evening blue light exposure delays sleep onset, fragments sleep architecture, and reduces overall sleep quality — even when total hours in bed seem sufficient.
For further reading, see: Harvard Health Publishing – “Blue Light Has a Dark Side.”
The result is a self-perpetuating cycle:
Poorer sleep → sustained HPA activation → elevated cortisol and low-grade inflammation → increased vascular permeability and fluid leakage → more pronounced under-eye puffiness and darker circles, due to increased visibility of subcutaneous blood vessels and shadowing.
Additional Physiological Contributors
Several secondary mechanisms further amplify under-eye swelling:
- Reduced lymphatic drainage — Restorative sleep supports efficient interstitial fluid clearance; sleep deprivation slows this process, allowing fluid to pool.
- Inflammatory response — Sleep loss elevates pro-inflammatory cytokines (such as IL-6), increasing capillary permeability.
- Dehydration compensation — Mouth breathing or reduced fluid intake during fragmented sleep can trigger compensatory fluid retention.
Evidence-Based Remedies and Prevention
The foundation of improvement remains sufficient sleep duration (7–9 hours) combined with early, consistent bedtimes that support full circadian alignment and restorative sleep phases.
Additional strategies include:
- Establishing a screen curfew 1–2 hours before bed (use night shift settings, blue-light-blocking glasses, or dim, warm lighting)
- Limiting dietary sodium intake (<2,300 mg/day) to reduce osmotic fluid retention
- Maintaining adequate daytime hydration
- Sleeping with the head slightly elevated (using an extra pillow) to minimize gravitational fluid pooling
- Applying cold compresses in the morning for temporary vasoconstriction and de-puffing
- Considering adjunctive therapies such as Manual Lymphatic Drainage (MLD) — a gentle, evidence-supported technique that enhances lymph flow, reduces localized edema, and activates parasympathetic relaxation
You can learn more about this service here: Facial Manual Lymphatic Drainage at Via Skincare
Persistent or severe under-eye swelling should be evaluated by a healthcare professional to rule out contributing conditions such as allergies, thyroid dysfunction, or other systemic factors.
Prioritizing both sleep quantity and sleep timing, along with minimizing evening blue-light exposure, remains the most clinically effective approach to restoring facial fluid balance, reducing periorbital edema, and softening the appearance of dark circles.




